Key Takeaways
- Dermatology medical billing errors are predictable and preventable.
- Revenue should flow through a pipeline, not cycle endlessly in rejections and resubmissions.
- Rooting out the causes of claim rejections is key for optimizing dermatology revenue.
- Find out how we’re improving medication management workflows.
If there’s one truth in practice ownership, it’s that you can’t care for patients if you can’t keep the lights on. No matter how committed you are to providing excellent care, your practice needs steady, reliable revenue to thrive. Taking the time to build a clear, intentional plan for billing and documentation sets your practice up for long-term success and helps you stay resilient through the ups and downs of business ownership.
Table of Contents
Rethinking the Revenue Cycle in Dermatology
Rather than thinking of your revenue as a cycle of rejections that come back to be resubmitted, envision it as a pipeline that flows cleanly with minimal friction. High-performing dermatology practices understand that high rejection rates are not an option. Prioritize your future, set financial KPIs, and aim for a streamlined billing pipeline where claims are clean, complete, and paid promptly.
Ask yourself:
- Are all services completely, correctly, and promptly billed?
- Are claims paid promptly and accurately?
- Do you know which services drive your revenue?
- If you can’t confidently say “yes,” it’s time to diagnose why.
Your dermatology billing system—whether managed in-house or through a partner—should be efficient, reliable, transparent, and accountable. Without these qualities, your system is vulnerable and prone to gaps and breakdowns that threaten your cash flow.
Reducing Claim Rejections in Dermatology Medical Billing
Claim rejection is the primary source of inefficiency in dermatology medical billing. The idea that insurers reject claims to hold back payments isn’t accurate; claims are typically processed without human intervention. Denials often happen due to avoidable errors, particularly in patient demographic entry and dermatology coding.
The root of many issues begins during patient intake. Collecting demographic and insurance information manually at check-in leads to lags in data and increases the chance of errors. Instead, your dermatology practice should:
- Enable patients to enter or verify their demographic and insurance details through your patient portal before visits.
- Use automated eligibility checks to confirm insurance status ahead of appointments.
- Address eligibility issues before the patient arrives to avoid payment delays.
- Schedule prior authorizations in advance for procedures that require them.
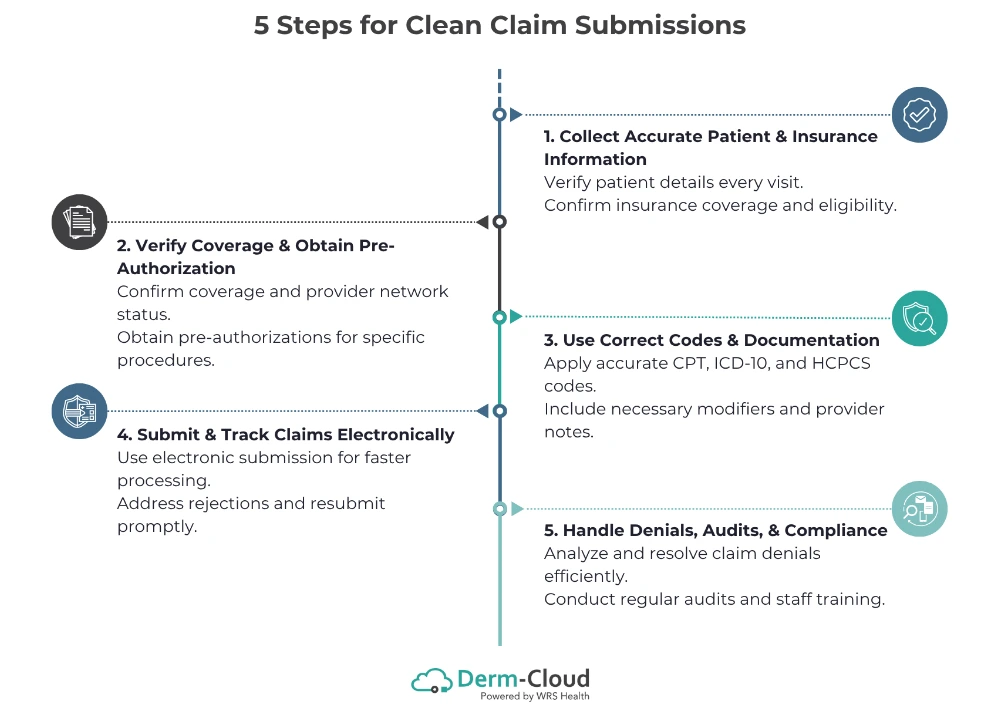
Clean Claims Through Accurate Dermatology Coding
The next step is ensuring claims are clean. A clean claim has complete and accurate information, with all needed documentation included. It uses correct medical coding and meets submission guidelines so it can be processed without delays. Every practice must review and eliminate reasons for rejections systematically by:
- Understanding local coverage guidelines.
- Using modifiers accurately.
- Pairing the right supportive diagnoses with services.
Your team should be trained in dermatology coding best practices to prevent recurring mistakes. Most dermatology practices provide a predictable set of services, making it easier to build efficient, repeatable billing workflows that prevent errors.
Claim rejections aren’t random. By addressing their root causes, your dermatology medical billing pipeline will flow smoothly, reducing friction and improving revenue stability.
Staying Consistent for Long-Term Stability
Improving your billing operations is not a one-time fix. Regularly reviewing your claim data, monitoring your key performance indicators, and addressing any trends in rejections or delays will help your practice stay ahead. Encourage your team to bring forward questions and ideas for improvement, and consider periodic training to keep everyone aligned with current coding and documentation best practices. These steady, small steps can add up to a stronger, more resilient practice that is prepared for whatever revenue challenges may come your way.
Partnering for Efficient Dermatology Billing
You’ve worked hard to build a practice that serves your patients with skill and care. Finetuning your billing processes keeps your practice healthy and lets you focus on your patients. Clear workflows, accurate dermatology coding, and proactive claims management build a financial foundation that helps you carry out your mission now and in the years ahead.
Managing your revenue can be draining, and sometimes bringing on a trusted partner makes a meaningful difference. Derm-Cloud’s specialized medical billing services and revenue management tools can help your practice reduce claim rejections, lower unnecessary costs, and strengthen your financial operations.
At the end of the day, taking small, consistent steps to improve your billing can help your practice stay steady while you continue doing the work you care about most: helping patients.